MYTH: There is no real payoff in engaging patients and families.
FACT: Health care organizations can reap many benefits from
“activated” patients and families – those who have the knowledge, skills and confidence to manage their own care.
How does engaging patients help? 1) It may increase quality of life by reducing falls, helping patients learn to manage chronic conditions. 2) It can reduce Underuse or Overuse of health services. 3) It may increases reimbursement through improved HCAHPS scores. And YOU may be more satisfied at work!
TWO EXAMPLES of positive results yielded from partnering with patients and families:
• One hospital that began involving patients and families in safety efforts after a highly publicized preventable death saw a culture shift that improved medication reconciliation and eliminated fatal medication errors during a 10-year period (Johnson & Abraham; Reinersten et al., 2008).
 • A health system that began seeking input from patients and families decreased nurse turnover from 15 percent to 5 percent in three years and improved patient, staff and physician satisfaction (Johnson & Abraham).
• A health system that began seeking input from patients and families decreased nurse turnover from 15 percent to 5 percent in three years and improved patient, staff and physician satisfaction (Johnson & Abraham).
WHAT CAN I DO TO ENGAGE PATIENTS? Listen to your patients to identify their level of activation in their care as described, & communicate in ways that move them to the next level.
level.
FOR MORE INFO, check out the source of above: Busting the Myths about Engaging Patients and Families in Patient Safety
CRITICAL THINKING: Think of a strategy that you ALREADY use or that you might start using to move patients up the stages of engagement in their own care. Be specific!



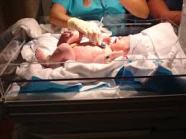 (Gray et al., 2006). About 12% of the 4 million born in U.S. hospitals were admitted to NICU’s. At birth every infant requires quick application of an armband, and when parents have not yet decided on a name the assigned name is often quite nondistinct (e.g., BabySmith).
(Gray et al., 2006). About 12% of the 4 million born in U.S. hospitals were admitted to NICU’s. At birth every infant requires quick application of an armband, and when parents have not yet decided on a name the assigned name is often quite nondistinct (e.g., BabySmith).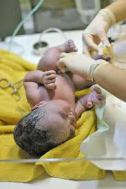 Their results? RAR events were reduced by 36.3%. Their recommendations? Switch to a distinct naming system.
Their results? RAR events were reduced by 36.3%. Their recommendations? Switch to a distinct naming system.


 Critical thinking: How would you apply
Critical thinking: How would you apply