So I’ve been pretty skeptical about people sewing protective face masks at home. And, as with a lot of things we don’t have all the data that we wish we had. So…I’m putting this scientific evidence out there and encouraging you to contribute to this blog by adding other scientific data.

Nevertheless, the expert opinion at CDC is that they are in the “Better Than Nothing” category and gives this additional advice. “In settings where N95 respirators are so limited that routinely practiced standards of care for wearing N95 respirators and equivalent or higher level of protection respirators are no longer possible, and surgical masks are not available, as a last resort, it may be necessary for HCP to use masks that have never been evaluated or approved by NIOSH or homemade masks. It

may be considered to use these masks for care of patients with COVID-19, tuberculosis, measles, and varicella. However, caution should be exercised when considering this option.1,2“
Anecdotally, providers are using them to extend the life of other masks or N95s. Women are also making some with little pockets for other filters, and a material called HANIBON that can be purchased online is used often on the outer layer of disposable masks and works to block out dust and fluids from entering.
References
- Dato, VM, Hostler, D, and Hahn, ME. Simple Respiratory Maskexternal icon, Emerg Infect Dis. 2006;12(6):1033–1034.
- Rengasamy S, Eimer B, and Shaffer R. Simple respiratory protection-evaluation of the filtration performance of cloth masks and common fabric materials against 20-1000 nm size particlesexternal icon, Ann Occup Hyg. 2010;54(7):789-98.
 “Sew” there you have it. Expert opinion is that as a last resort you may use inadequately tested cloth masks if it is all you have. I am grateful for all those sewists out there responding to medical center calls to supply them with cotton and elastic homemade masks, and sending out the patterns to do so. Field medicine.
“Sew” there you have it. Expert opinion is that as a last resort you may use inadequately tested cloth masks if it is all you have. I am grateful for all those sewists out there responding to medical center calls to supply them with cotton and elastic homemade masks, and sending out the patterns to do so. Field medicine.
CDC also says “The filters used in modern surgical masks and respirators are considered “fibrous” in nature—constructed from flat, nonwoven mats of fine fibers” If this is true then would nonwoven interfacing  improve the homemade masks?
improve the homemade masks?


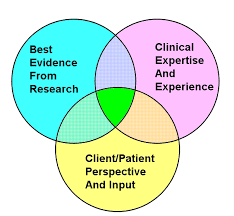 Practice based in evidence (EBP) means that you must critique/synthesize evidence and then apply it to particular setting and populations using your best judgement. This means that you must discriminate about when (and when NOT) to apply the research. Be sure to use best professional judgment to particularize your actions to the situation!
Practice based in evidence (EBP) means that you must critique/synthesize evidence and then apply it to particular setting and populations using your best judgement. This means that you must discriminate about when (and when NOT) to apply the research. Be sure to use best professional judgment to particularize your actions to the situation!



 Privacy
Privacy applications, such as maps and camera. The iOS version for the iPhone can access all Google data.
applications, such as maps and camera. The iOS version for the iPhone can access all Google data. Safety:
Safety: 
